Is CGM a fuel gauge?
- Asker Jeukendrup and Mike Riddell
- Sep 27, 2023
- 6 min read
Updated: May 4
Wouldn’t it be great to have a tool that measures how much fuel is left in your tank, just like a car has a fuel gauge? This would allow you to make sure the tank is full at the start and you can top it up before it runs out. Maybe there even is an optimal fuel level for performance? In the previous blog, we discussed CGM (Continuous glucose monitoring) sensors that have now become available to many athletes. Could CGM be the fuel gauge athletes have been waiting for?

What CGM can (and cannot) measure
The body only holds a few grams of glucose in circulation, only about 4-5 grams, but this is a critical fuel source for skeletal muscle, the brain, and the nervous system. Since blood glucose is an important fuel for the muscle, particularly for prolonged exercise at a moderate to high intensity, it is an attractive idea that measurements of glucose in real-time with CGM could be used as a “fuel gauge” or “carbohydrate sensor”.
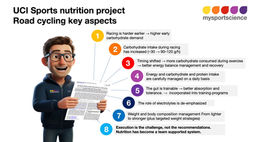
As we will discuss in this blog, this is an oversimplification. Blood glucose is just one source of fuel of the muscle. As can be seen in the infographic, carbohydrates (glucose) used during exercise will come from muscle and from blood (and the glucose in blood will come from storage in the liver or from the intestine after carbohydrate intake). The glucose stored in the muscle (called glycogen) is a critical fuel source and it will not appear in the circulation (blood). Any glycogen stored in the muscle (up to about 800g) cannot escape from the muscle into the blood.
CGM can’t measure glycogen in the muscle. So, when we measure blood glucose (or interstitial glucose) we are only measuring glucose from the liver and intestine (absorption), but it does not give us information about the muscle glycogen content. However, even when CGM doesn’t directly measure muscle glycogen it could still act as a sensor for carbohydrate availability, IF the glucose in the interstitial space would always change in parallel with changes in muscle glycogen. Although there are situations where this might be the case (for example during prolonged exercise without food), there are also (many) situations where this is not the case. It is possible to have high muscle glycogen and low blood glucose, or low muscle glycogen with very high blood glucose concentrations.
CGM can't measure glycogen in the muscle. So, when we measure blood glucose (or interstitial glucose) we are only measuring glucose from the liver and intestine.
Contribution of blood glucose to total fuel use
The higher the exercise intensity, the more blood glucose will be used, but it still only contribute roughly 20-30% to the overall fuel use. During lower intensity exercise, fat is usually the most important substrate and during high intensity exercise muscle glycogen becomes the dominate energy source. The contribution of muscle glycogen is even more dependent on the exercise intensity: It can be minimal, but it can also be 80% of all fuel.
Changes in glucose concentrations from CGM
For most athletes, when they wear a CGM at rest and during exercise they typically find that the glucose ranges from about 90 mg/dL to about 120 mg/dL (or 5.0 mmol/L to about 6.7 mmol/L). After eating a meal rich in carbohydrates that are rapidly absorbed, like sugar cereals and white rice, users of CGM will notice that their glucose will also rise transiently, sometimes exceeding the range 90-120 mg/dL. This is a normal physiological response.
In healthy individuals not living with diabetes, glucose concentrations are pretty tightly regulated within this range. Sometimes there is a short period where glucose concentrations drop below this or go above these values.
For example, during high intensity exercise, glucose concentrations can rise significantly (sometimes to over 140 mg/dL), but this is not because there is more use of blood glucose but rather there is more production of glucose by the liver and the muscle is predominantly using glycogen as its fuel source. So, glucose tends to rise.
Glucose concentration and glucose flux are not the same
Measuring the concentration of glucose, as with a CGM, is not the same as measuring the flux of glucose from one organ to another or from cell to cell. To illustrate that glucose concentration can be quite different than the actual supply of fuel to the muscle, see the figure below:

This analogy with a bucket shows the difference between a concentration and glucose uptake or glucose flux. The buckets is our circulation and the level of water in the bucket is blood glucose. There is a hole in the bucket and the water flowing out of the bucket through this hole represents uptake in tissues (muscle and brain for example). At the same time, we also pour in new water (this represents glucose coming from the liver). As long as we pour in exactly the amount that disappears into tissues the concentration (the level of water in the bucket) will stay the same.
On the right, the hole in the bucket is larger. More glucose is disappearing into tissues (for example during exercise as the need for fuel is increased). The liver then produces more glucose so that the concentration stays the same. So, we have two situations with similar blood glucose concentrations but a large difference in glucose uptake and glucose production. There is a much larger “flux”. This indicates that if we just measure a concentration, it does not tell us much, if anything, about glucose use.
Glucose and the brain
It is not just about providing the muscle with fuel. Blood glucose is the most important fuel for the brain. The brain is much more dependent on glucose as a carbohydrate source. When blood glucose supply to the brain is low, several symptoms develop (nausea, dizziness, weakness, tremor, shivering, confusion, disorientation, cold sensations, etc). In general, mild hypoglycemia can be defined as a blood glucose or sensor glucose value of <70 mg/dL (or <3.9 mmol/L) with lower values typically giving more exaggerated symptoms.
However, not everyone will experience symptoms even at fairly low blood glucose concentrations. On the other hand there will be individuals that have mild symptoms at relatively high glucose levels. When hypoglycemia occurs after prolonged exercise (during a long bike ride or run for example), it generally means that the exercise intensity and/or performance drops and we refer to this as hitting the wall or bonking. There are some spectacular examples in sport where athletes seem to be performing well one moment and come to a near standstill the next.
Sure, ingesting carbohydrates when this occurs can help, but it’s already too late as far as peak performance is concerned. It would be better to have prevented this altogether. If a CGM could help to detect this early this could then trigger carbohydrate intake in a more strategic fashion. With measurements of glucose every minute and a device that indicates your glucose directional trend (i.e., it’s starting to drop towards hypoglycemia, but you are not there yet!), it will help to prevent such situations. This is one strategic use of CGM in sport.
CGM can detect your glucose directional trend, allowing you to see glucose drop towards hypoglycaemia during exercise, even if you are not there yet.
Summary
In summary, like any technology, CGM has its uses but also its limitations and optimal use of the technology means you need to understand both the possible benefits as well as the limitations. What we measure in blood or interstitial fluid with a CGM is at best a very insensitive fuel sensor. This does not mean that CGM is not useful, it just has limitations on what we can interpret from the data. It appears that a CGM can help to detect hypoglycemia before it is too late and tell an athlete to eat before it is too late. There are several very useful applications we will discuss in the next blogs.
This blog post was co-written with Professor Mike Riddell, PhD from the Muscle Health Research Center, York University, Toronto, Canada.
Disclaimer: Asker Jeukendrup is a consultant to Supersapiens. Michael Riddell serves as a scientific advisor to Supersapiens and as a consultant to Dexcom Inc, another CGM device company.